Back Pain
Back Pain Specialists
What Causes Back Pain?
Back pain can develop for many reasons. Some of the most common conditions we evaluate and treat include:
✅ Spinal Stenosis
✅ Sprains and Strains
✅ Arthritis
✅ Degenerative Disc Disease
✅ Herniated Discs
✅ Radiculopathy and Sciatica
✅ Muscle Spasms
✅ Piriformis Syndrome
✅ Scoliosis
✅ Spondylolysis
Back Pain Specialists
What Causes Back Pain?
There are many various causes of back pain or referred back pain, but some of the most common origins that we find and treat are:
✅ Spinal Stenosis
✅ Sprains and Strains
✅ Arthritis
✅ Degenerative Disc Disease
✅ Herniated Discs
✅ Radiculopathy and Sciatica
✅ Muscle Spasms
✅ Piriformis Syndrome
✅ Scoliosis
✅ Spondylolysis
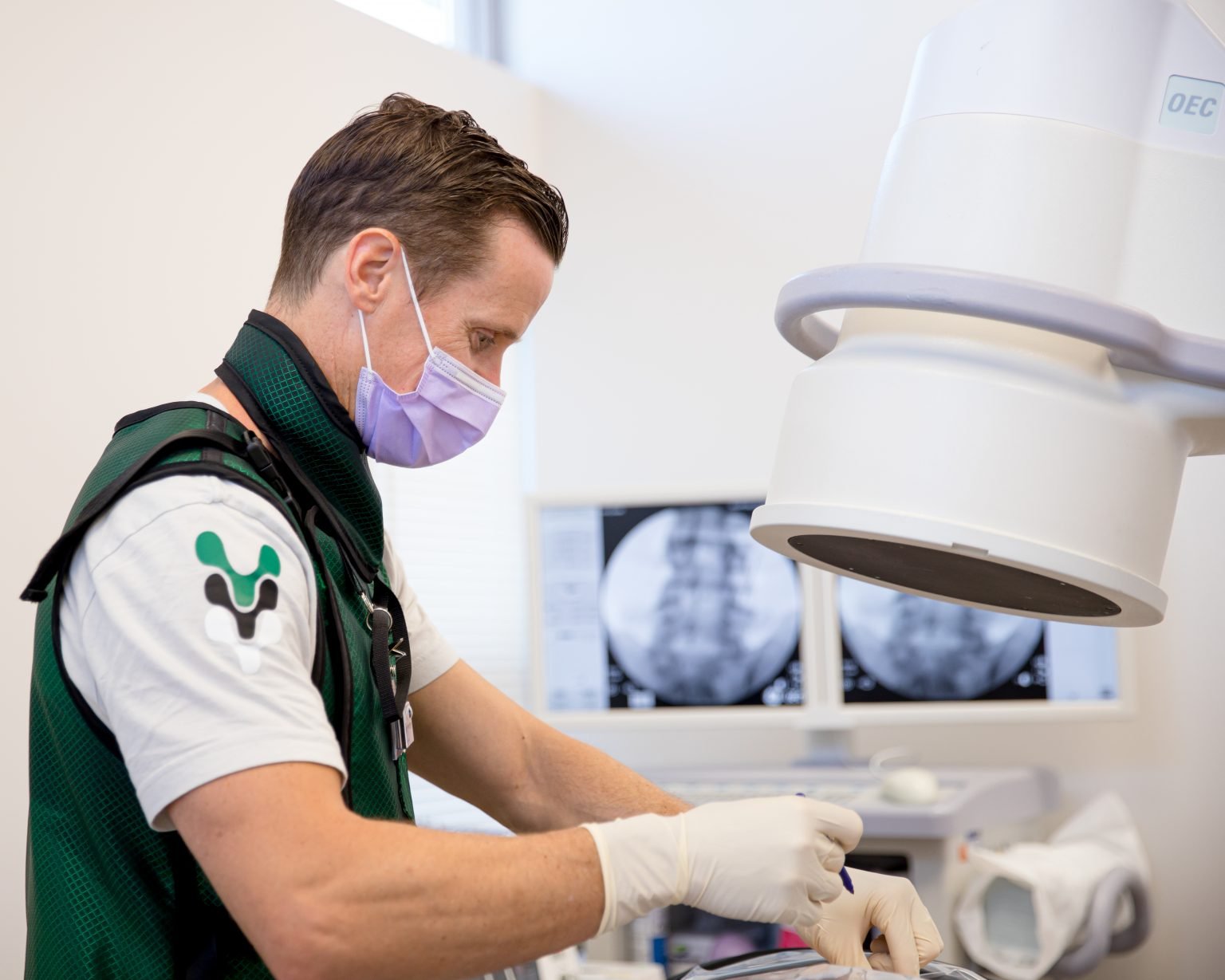

PA Pain & Spine Institute
Back Pain Specialists in Chalfont & Quakertown
At PA Pain & Spine Institute, our back pain specialists evaluate and treat spinal conditions that affect daily life. From acute injuries to chronic conditions, we provide personalized, minimally invasive treatment options designed to help improve mobility, reduce pain, and support long-term function.
Signs and Symptoms of Back Pain Conditions
Signs and Symptoms of Back Pain
Back pain may appear suddenly after an injury or develop gradually over time. Common symptoms include:
- Ongoing or worsening back pain
- Pain that radiates to the leg, foot, arm, or hand
- Numbness or tingling
- Muscle weakness
- Pain that interferes with sleep, work, or daily activities
If your symptoms are persistent or worsening, professional evaluation may be appropriate.
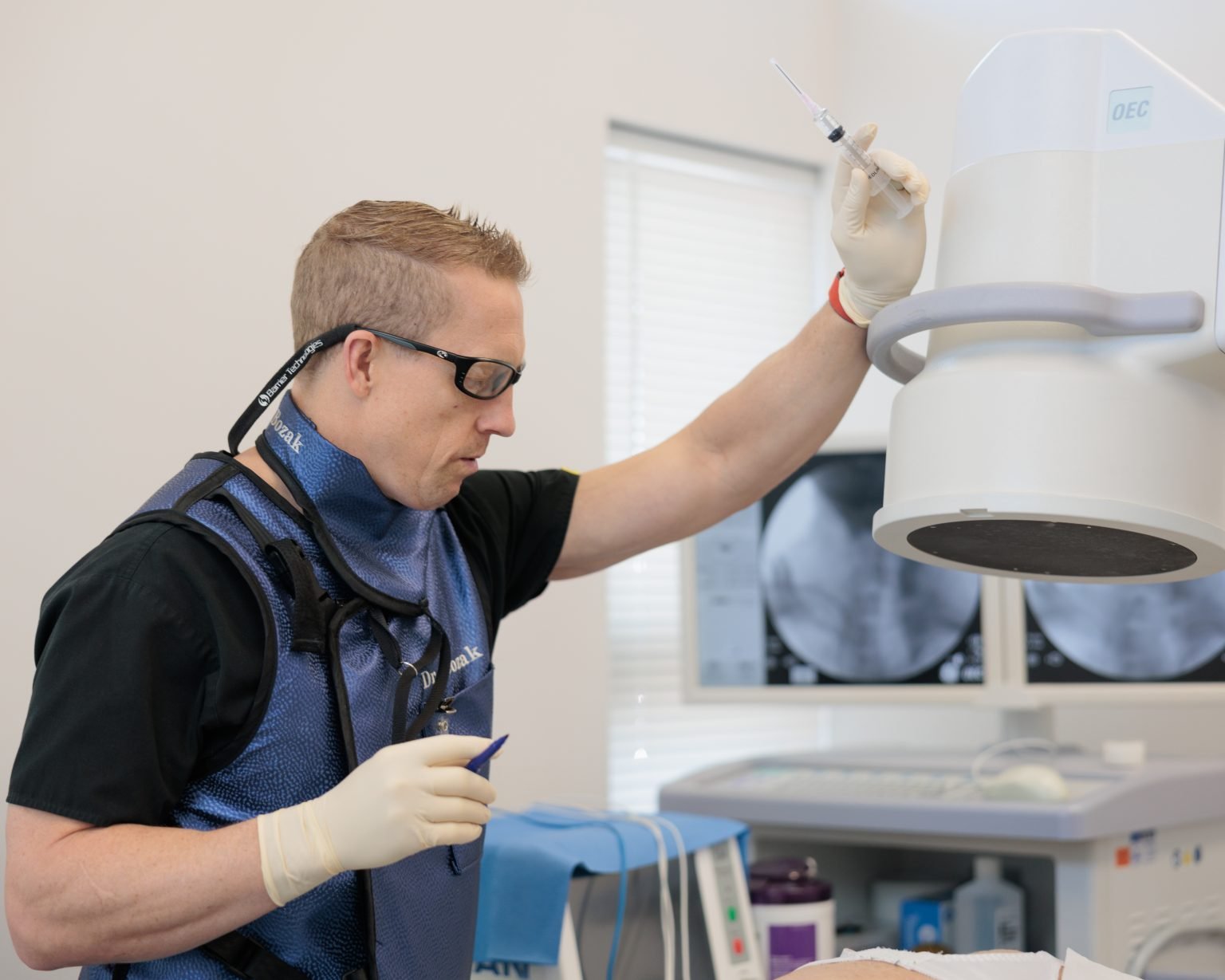
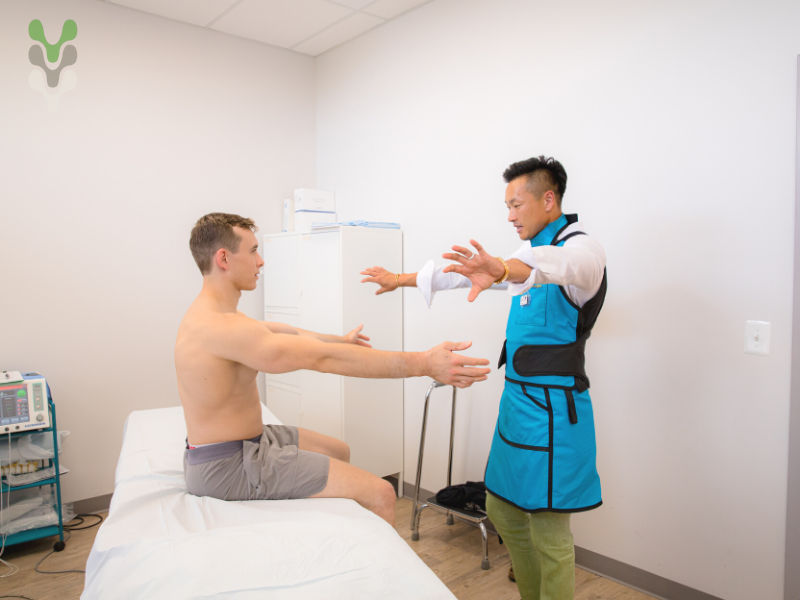
Our Comprehensive Approach to Back Pain Diagnosis
We begin with a thorough evaluation to better understand the source of your pain. This may include:
- Review of medical history and prior treatments
- Physical and neurological examination
- Imaging such as X-rays or MRI (when clinically indicated)
- Nerve studies or diagnostic injections (when appropriate)
This process allows our specialists to create a personalized care plan based on your condition and goals.
Back Pain Treatments
Treatments can vary based on pain origin and other related conditions, but in general some of our minimally invasive, effective back pain treatments are listed below.
Spinal Injections
Spinal injections, such as an epidural, are done under fluoroscopy guided imaging for accuracy and inject anesthetics or anti-inflammatory medications near the affected nerve area(s) for inflammation reduction and pain relief.
*This is done outpatient and does not require anesthesia.

Nerve Blocks
Nerve blocks are fluoroscopy guided injections that target specific clusters of nerves associated with the area of pain with a 'blocking' or numbing medication to help stop or block the pain sensations sent throughout that area of the body.
*This is done outpatient and does not require anesthesia

Radiofrequency Ablation
This minimally invasive procedure utilizes fluoroscopy guided imaging to target the medial or lateral branch nerves that are sending pain signals from various joints. The needle tips are placed in these areas and are connected to electrodes to pass small amounts of electrical currents and heat that target the nerves to allieviate the nerve sensations.
*This is done outpatient and does not require anesthesia

Muscle + Tendon Injections
Muscle and tendon pain/inflammation is treated using trigger point injections which inject a small amount of anesthetic or steroid medication for pain relief. Tendon pain is often treated by ultrasound guided injections with pain-blocking medications for localized relief.
*This is done in clinic and is similar to receiving a normal shot at a doctor's office.
Spinal Cord Stimulation
This mini-surgical procedure is done on a trial basis prior, and it is aimed at providing consistent nerve pain control and relief. Electrical leads are placed into the epidural space of the spine to trigger various pulsations to the surrounding nerves in various ways to provide relief and promote mobility. These pusling sensations are controlled via a blue tooth remote and have the ability to be adjusted as needed.
*This is done outpatient and does not require anesthesia.
Regenerative Therapies
In the event that tissue, cells, or nerves are damaged some regenerative therapies can be effective in the rebuild and regrowth of the damaged area. Utilizing your own healthy blood or donated cells to inject damaged areas help to accelerate the repair process.
*This is done outpatient and does not require anesthesia.

Minimally Invasive Lumbar Decompression (MILD)
This minimally invasive procedure is used to treat Spinal Stenosis. It is performed in a surgery setting with a tiny incision to remove the stenosis and open up the spinal canal to provide relief.
*This is done outpatient and does not require anesthesia.

Intrathecal Pump Therapy
This minimally invasive procedure is surgically performed to place a programmed pump with pain medication into the back in order to consistently control the pain when other therapies have not worked.
*This is done outpatient and does not require anesthesia.

Kyphoplasty
This surgical procedure treats Vertebral Compression Fractures through careful expansion and stabilization of the spine's vertebra.
*This is done outpatient and does not require anesthesia.
Medication Management
In conjunction with other treatments, medication can be a helpful tool in managing pain. Medications such as anti-inflammatory, steroids, medical marijuana, etc. may be options depending on your condition.
When Should You See a Doctor?
You may want to schedule an evaluation if you experience:
- Back pain lasting more than several days
- Pain that does not improve with rest or home care
- Recurring episodes of back pain
- Numbness, tingling, or weakness in your arms or legs
- Pain that limits daily activities
Seek urgent medical care for severe pain following trauma, pain with fever or signs of infection, changes in bladder or bowel function, or rapidly worsening weakness or numbness.

FAQs
What Causes Back Pain?
The spine is a complex structure of bones, muscles, ligaments, and nerves that work together to support your body and enable movement. When any component is injured or degenerates, it can result in significant pain and disability. Understanding the various causes of back pain helps our specialists develop targeted treatment approaches.
Spinal stenosis occurs when the spinal canal narrows, putting pressure on the nerves that travel through it. This condition often develops gradually and causes pain that worsens with walking or standing. Herniated discs happen when the soft center of a spinal disc pushes through its outer ring, potentially pressing on nearby nerves and causing intense pain. Degenerative disc disease involves age-related wear and tear of the spinal discs, leading to reduced cushioning between vertebrae
Radiculopathy and sciatica result from nerve compression, causing pain that radiates along the path of the affected nerve. Arthritis can affect the joints in the spine, causing inflammation and stiffness that limits movement. Spondylolysis involves stress fractures in the vertebrae, often seen in athletes or people who perform repetitive back motions.
Scoliosis creates an abnormal curvature of the spine that can cause pain and breathing difficulties in severe cases. Vertebral fractures, whether from trauma or osteoporosis, can cause sudden, severe pain and require immediate attention. Failed back surgery syndrome occurs when patients continue to experience pain following spinal surgery, often due to scar tissue formation or incomplete healing.
Soft tissue problems also contribute significantly to back pain. Sprains and strains involve injured ligaments or muscles, typically from sudden movements or overexertion. Muscle spasms create involuntary contractions that can be extremely painful and limiting. Piriformis syndrome occurs when the piriformis muscle compresses the sciatic nerve, causing pain that mimics disc problems. Myofascial pain syndrome involves chronic pain in muscle trigger points that can refer pain to other areas.
Who is at Risk for Back Pain Related Conditions?
While back pain can affect anyone at any age, certain factors significantly increase your risk of developing chronic spinal conditions. Understanding these risk factors can help you take preventive measures and seek early treatment when necessary.
Age naturally increases your risk as the muscles and connective tissues in your back become less flexible and more prone to injury over time. The spine itself undergoes degenerative changes, including disc compression and joint wear, which can lead to chronic pain conditions. However, age alone doesn’t guarantee back problems, and many older adults maintain healthy, pain-free spines through proper care.
Lifestyle factors play a crucial role in back health. A sedentary lifestyle with prolonged sitting weakens the muscles that support your spine and increases pressure on spinal discs. Poor posture habits, whether from desk work or daily activities, create imbalances that stress certain parts of your spine while weakening others. Lack of regular exercise and core strength leaves your spine without adequate muscular support.
Obesity or excess weight puts additional stress on your spine, particularly the lower back, accelerating wear and tear on joints and discs. Physically demanding occupations involving heavy lifting, repetitive motions, or prolonged standing increase injury risk, especially when proper body mechanics aren’t used. Previous back injuries or surgeries can create weakness or instability that predisposes you to future problems.
Smoking significantly impacts spinal health by reducing blood flow to spinal tissues, impairing healing, and accelerating disc degeneration. High stress levels contribute to muscle tension and can worsen pain perception. Poor sleep quality affects your body’s ability to heal and repair tissues, while also lowering your pain threshold.
Certain medical conditions also increase back pain risk. A family history of spinal conditions suggests genetic predisposition to disc problems or spinal deformities. Osteoporosis weakens bones and increases fracture risk, while autoimmune conditions like rheumatoid arthritis can affect spinal joints and surrounding tissues.
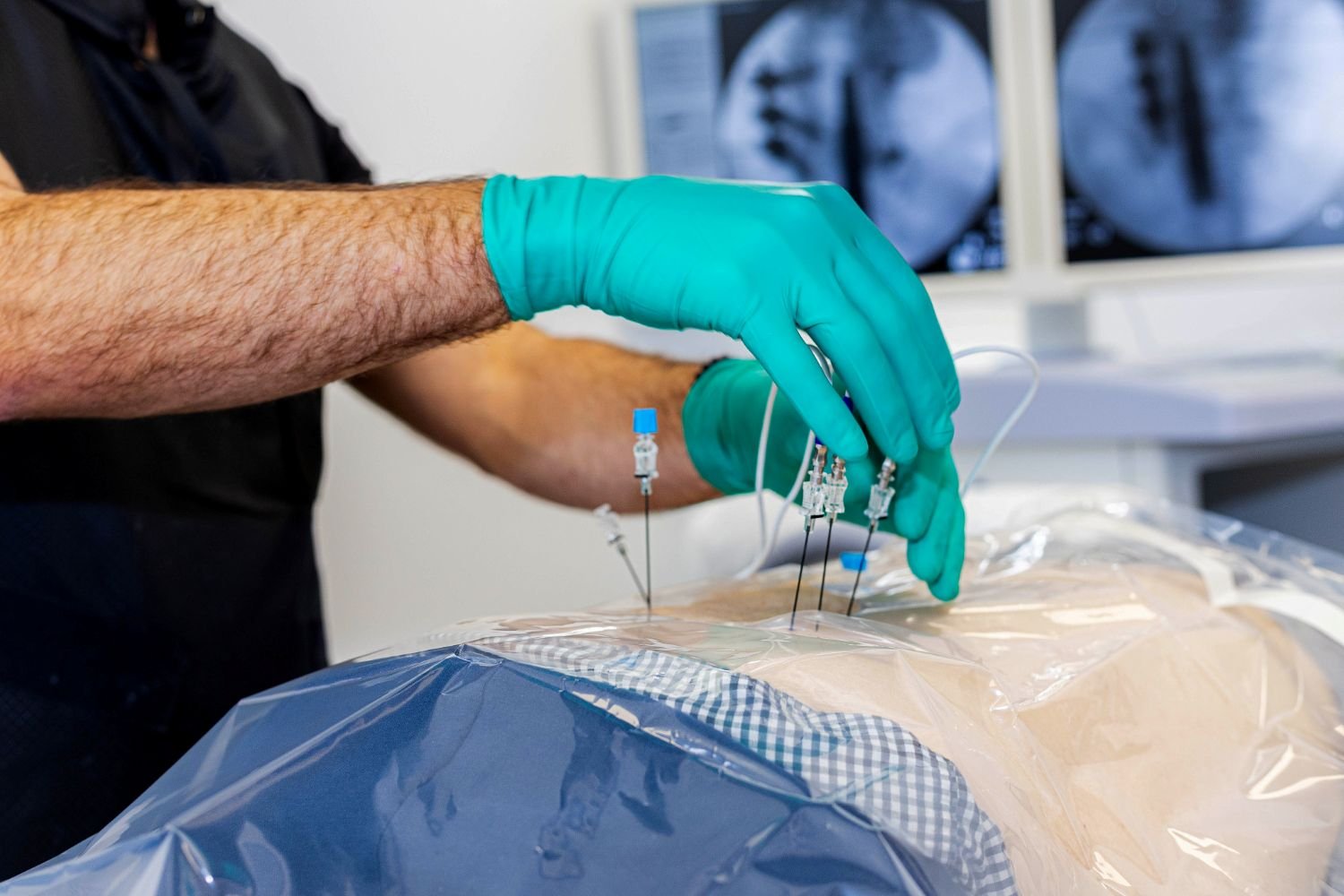
Why Choose PA Pain & Spine Institute?
Our board-certified pain management specialists provide personalized, patient-centered care using a conservative-first approach with minimally invasive treatment options at convenient locations in Chalfont and Quakertown.
Take the First Step Toward Evaluating Your Back Pain
Back pain can be disruptive and frustrating. Our team is here to help you understand your options and create a treatment plan tailored to your needs and lifestyle.